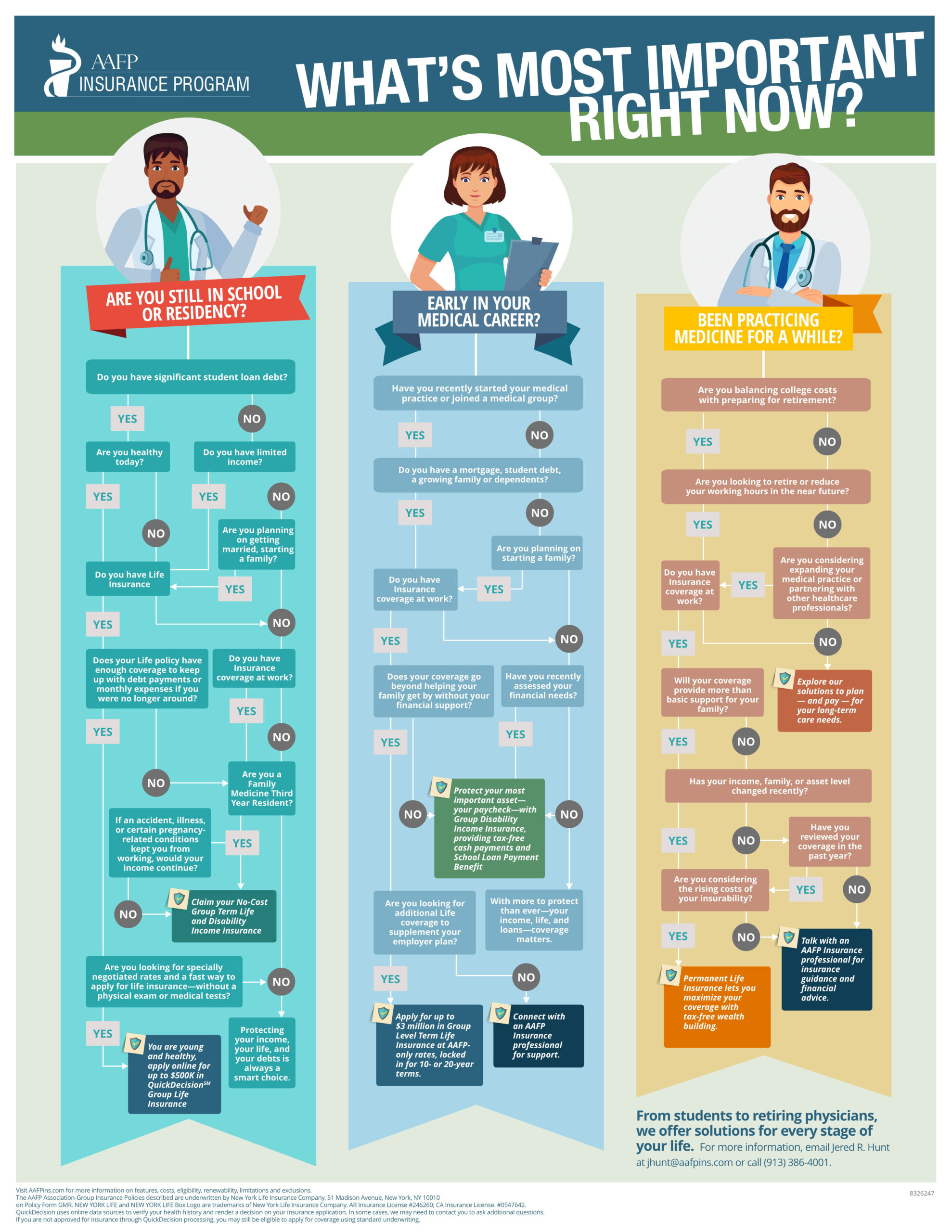
What’s the difference between concierge medicine and direct primary care?
The main reason for all the confusion surrounding DPC and concierge medicine is that the concept of operating a medical practice that does not bill services through an insurance company is still new. And with these two models emerging in the healthcare marketplace, there is a lot of misinformation floating around.
To clear the air, here are some of the basic differences:
- Practices that operate under the DPC practice model charge an average of $77 per month in membership fees; concierge practices often charge higher fees – in the ballpark of $183 per month, according to a research article by the AAFP.
- The traditional form of concierge medicine involves the patient paying a monthly or annual fee in exchange for direct access to a physician. While the practice profits from these membership fees, they also bill insurance companies for visits. However, under the DPC model, many providers do not accept insurance whatsoever, and solely rely on the monthly/annual fee they receive from their patients.
Under both models of care, physicians benefit from being able to keep their patient numbers small and can spend more quality time treating patients – generally 35 – 45 minutes, compared with eight minutes in the current model.
Another key distinction between the two is that direct primary care is explicitly mentioned in the Affordable Care Act as an acceptable option for receiving medical care without insurance, while concierge medicine is not.
Pros and cons of each care model
Each model of care has its advantages and disadvantages. Let’s start with concierge medicine:
From the financial side of life, concierge practices may collect money from two revenue streams: membership fees and insurance payments, and thus not be as concerned with fighting insurance companies as they would in a traditional medical practice.
One downside to concierge practices comes from those physicians who still accept Medicare patients. Providers are subject to those government regulations for payment such as meaningful use guidelines.
On the flip side, the key benefit to direct primary care is that these practices are not subject to Medicare regulations. They also don’t have to concern themselves with contracting with insurance companies, or worry about claim denials, pre-certification, collecting co-pays, etc.
There is one drawback: DPC practices only have one source of revenue and that is strictly from the patient. That means practices must remain diligent with their financial planning to ensure patient fees are enough to support practice operations.
What does the average DPC/concierge medicine patient look like?
In the beginning, concierge medicine was exclusive to wealthy patients who could afford to have round-the-clock access to top medical professionals. The most attractive feature: house calls. Now that times have changed, concierge medicine is drawing in a different crowd.
Middle income patients and those on Medicare and Medicaid benefit the most from DPC/concierge medicine services due to costs and a more personalized medical experience. The membership fees combined with a high-deductible health plan is often still cheaper than traditional insurance. This is especially helpful for patients who suffer from chronic illnesses and make multiple doctor visits.
In a survey conducted by the Concierge Medicine Research Collective, they found that people age 50 and older make up an increasing share of patients at most concierge practices. As a result, concierge practices tend to be concentrated in states with higher populations of older adults, such as California and Florida.
Is concierge medicine or direct primary care right for you?
There’s no denying the high level of interest in these two new models of care. The AAFP estimates 2 percent of its 68,000 members offer direct care. And in a paper by the American College of Physicians, they estimate between 1.3% to 9.6% of primary care physicians have converted to concierge medicine, or are moving toward them with “hybrid” models.
With the increase in popularity, some physicians may consider making the switch. But there are some important factors to keep in mind, particularly for young physicians.
First, you will need to consider how the transition to direct primary care or concierge will affect your patients. This is one of the most challenging aspects of opening a solo practice based on these models because you will have to drastically cut your patient load.
In addition, while the fees are generally cheaper than paying monthly insurance premiums, some lower-income patients may still have difficulty paying for the medical care they need.
Next, you’ll need to decide if you want to offer certain features such as telemedicine visits, 24/7 cell phone access, weekend hours or house visits. This will help determine how much extra work you’re willing to do outside of the office and how much you plan on charging patients for these added benefits.
Lastly, you’ll need to do a significant amount of financial planning since there will be large upfront investment in getting your practice off the ground. It’s a risky decision and one that shouldn’t be made lightly. It’s important that you consult with colleagues or other physicians who have successfully made the transition as well as a financial advisor to help manage your investment.
Whether you’re considering direct primary care or concierge medicine, it’s crucial to keep in mind why you want to make the switch. The idea is that doctors who no longer want to jump through hoops with insurance companies can now focus on treating their patients. With less time spent on administrative duties, you can provide care that’s more personal and convenient than in other practices.
Tell us: Are you considering moving your practice to DPC or concierge? If so, why, and what steps have you taken to make the transition?
Photo Credit: Shutterstock